
A 24-hour unannounced visit to the St Ann’s Bay Hospital by a Sunday Gleaner news team has revealed a litany of woes, which suggests that the Type B facility might be sicker than the scores of patients who seek treatment there daily.
The hospital is bursting at the seams with an increase in patient load following the current outbreak of chikungunya, but that is not the main concern of most persons who visit the facility.
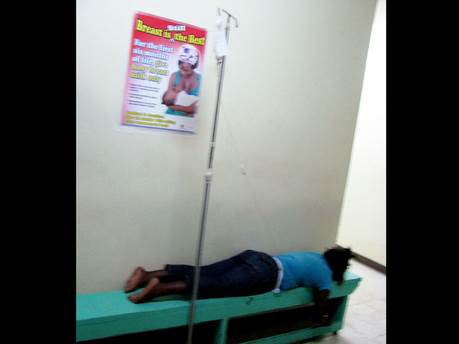
With many patients forced to make do with benches and the floor as beds in the severely overcrowded facility, some charge that this is not their greatest concern.
Instead, it is the treatment meted out to them by medical personnel and the shortage of critical material, which the patients say, are posing the greatest challenges.
Having entered the facility with no hassle, the incidents observed in the relatively short period underscored much of what is wrong at the hospital.
At one point, a woman in a wheelchair, who seemed badly in need of care, was left unattended for a significant period until she fell to the floor, wallowing in her own vomit. Only then did a nurse and a security guard attend to her.
Later, a man who entered the accident and emergency area with what appeared to be a chop wound, stumbled and fell. He charged that his hand was broken in the fall. However, a nurse said she could not help him at the moment as there were no splints, so she would need to make one and did not have the time to do so. Another nurse asked how he had broken his hand, and following his response, she hissed her teeth and walked away.
Stunned by the two incidents, our news team was faced with a woman who alleged that a bus had run over her foot, causing her great pain. She charged that the doctor who examined her said nothing was wrong with the foot and gave her no medication despite the pain she was feeling.
Another woman, who was waiting to be screened in the outpatients department, fainted before she was attended to, and other patients told similar tales of horror. One man charged that his daughter had been in an accident on a Wednesday, but when she visited the hospital, a doctor told her to return the next day as she would not get through for that night.
A 44-year-old renal patient, who spent five days on the male medical ward, said: “The treatment isn’t bad, but the stench and flies. Plus, that’s where they have the men that are sick in their head locked up in a cage. They all fight one another and the noise mek yu all sicker than how yuh go in.”
In the wee hours of the morning when patients would be expected to be asleep, activity among the staff seemed high. At 2:10 a.m., a female doctor started shouting a patient’s name. She then walked to the door to make one final call before making a hissing sound and saying, “I
don’t see why I should be walking looking for anybody.”
At 2:50 a.m., a nurse started pushing a squeaky table across the room. Less than one hour later, a male patient started calling loudly for the nurse to assist him to the bathroom. With no help, he decided to go it on his own and was told to return to bed, where he wet himself. By 4:15 a.m., the patients were being awakened as it was time for them to be ‘tidied’.
SURPLUS OF PATIENTS
On the other side of the coin, medical personnel complained that the hospital was facing a shortage of supplies and staff, leaving them almost impotent in catering to the needs of the influx of patients who visit the institution daily. They said this had been compounded by the chik-V outbreak.
According to a medical source at the hospital, it is short of sterile gloves, sutures, non-rebreather masks, oxygen masks, nebulisation chambers, and masks, among other critical supplies.
But Leon Gordon, chairman of the North East Regional Health Authority, said the shortage of some supplies was not unique to the St Ann’s Bay Hospital.
“I’m not going to say that things don’t run out, of course you can run out, but the hospital is not the only place to run out of things,” said Gordon.
“You run out of things sometimes because of the high usage, and there can be some lapses somewhere in terms of ordering and delivery process. But is it that you will remain without it or you take steps to replenish? That is the key question,” added Gordon.
For senior medical officer at the facility Dr Nicole Dawkins, the hospital is facing unusual pressure at this time.
“What has come up is the flood, which is a month earlier than normal. Normally, what we would have done is beef up things in November, with the expectation of the December rush, so what we have to do is beef up things now, which is what we have started doing,” said Dawkins.
“We have started peaking in September, which is unusual, because normally, we don’t start peaking until November,” added Dawkins.
She said that the overcrowding and resultant strain on hospital resources could be avoided if people with non-critical illnesses sought care at health centres.
The St Ann’s Bay Hospital serves at least three parishes, with an average bed complement of 139, but with the rush, some patients are left to their own devices.
During the visit by our news team, patients were witnessed setting up makeshift beds on benches and chairs, while some just went without sleep. One patient quipped that it would have been better in a morgue as “at least you would get your own space”.
A woman who had had a miscarriage managed to soldier on for the duration of her stay at the hospital. “I didn’t sleep at all last night as there was no bed. I had to sit up for the night.”
Dawkins argued that the problem was not with the number of beds, but the limited space in which to situate them, plus the patients who remained at the hospital after being discharged.
“It is not a bed issue; it is a ward space issue, which is why we had a ward expansion. It has not remedied the issue totally because there are still other issues as it relates to the use of beds. Up to this morning, we had about 12 patients who have been discharged but have not gone home. So that’s one set of beds that is not turning over fast,” said Dawkins.
In the meantime, one man, who claimed he had been at the hospital since 7 a.m. on Wednesday, was not seen by a medic until 5 a.m. Thursday, at which time he was admitted. He was seen leaving the hospital not long afterwards, claiming: “I don’t nyam weh dem a serve in deh.”
The quality of food at the hospital was a major complaint of several of the patients and one that the SMO did not dismiss.
“We don’t have a decent canteen, so if patients are not on a strict diet and they don’t want what is provided, they have the option to get their own. We … have some vendors on the outside who are selling more variety than we, so we allow them (patients) to go out and come back,” explained Dawkins.
[email protected]

This is a disgrace. ..
Not even Jamaica hospital in the 60s was like dis. Come on man, no excuses fi dis level a fckry.
(Heavy sigh) A who mi did hear seh poverty is a crime? Mus be because nuh suffer dem patients deh a suffer pon top a dem ailments? let me start with the minister of health where’s s/he? Not even a mangy dog fi get tratment deh so. Nurse a kiss r teet, so much for caring and compassion. A whole 24hrs later b4 ur seen. The serving of insipid food, broken chairs, the lack of basic supplies. Portia go tek a tour in a u backyard u nuh need fi go overseas pon a nex tour. I am pissed to say the least reading this.
Folks im kinda neutral on this one, jamaica have way more population now than then so most likely more people ago want health care. government cant duh nuh better on this one. one thing to note them CAN mek beds locally for the hospitals though. jamaica nuh have nuh economy fi dem can assist them in anyway.
Help
I am from St Ann and its a shame and disgrace, I wouldn’t even want my enemy to be treated like that. Heath care is a basic human right. The government should use our tax dollars better.